The Future of Humanitarian Surgery: From Intervention to Partnership.
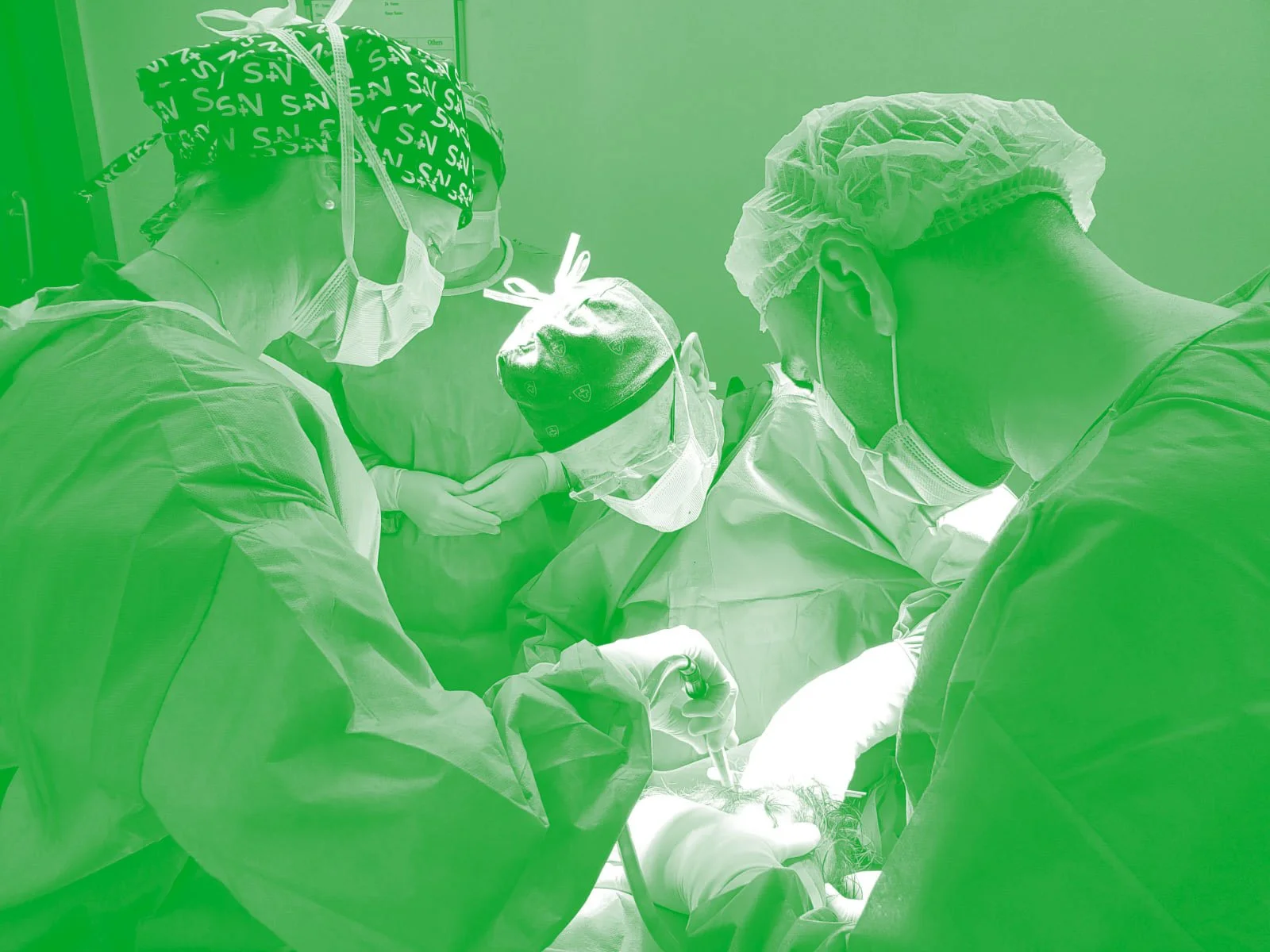
Partnerships in practice: international volunteer medical surgeons working hand in hand with local practitioners in Erbil, Kurdistan, Iraq.
In many parts of the world, access to safe, timely, and affordable surgical care remains out of reach for millions. Humanitarian surgery has long stepped in to fill urgent gaps—often through humanitarian missions led by international teams. These efforts have saved and transformed lives.
However the future of humanitarian surgery must evolve into something more enduring: a system that is sustainable, locally led, and strengthened through global collaboration. At Swisscross, this transition is not theoretical—it is already being practiced.
Rethinking the Traditional Model
For decades, humanitarian surgery has relied on rapid deployment: international teams arrive, perform operations, and leave. While impactful, this model creates structural limitations:
Fragmented follow-up care
Limited transfer of knowledge
Dependence on external actors
Minimal long-term system strengthening
The next phase of humanitarian surgery must move beyond volume and urgency toward continuity, resilience, and local ownership.
The Swisscross Model: Efficient, Effective, and Empathetic Care
Swisscross has developed a model that reflects a deeper evolution in humanitarian healthcare—one built not only on clinical excellence, but on efficiency, collaboration, and empathy.
At the core of the Swisscross model is a belief that the future lies in collaboration between specialized, “niche” actors rather than isolated efforts. As Swisscross founder and Chair Dr. Enrique Steiger emphasizes, humanitarian impact increases when organizations share expertise, resources, and responsibility rather than compete for them.
This approach allows, more patients to be treated at lower cost, greater coordination across organizations and a unified response to complex surgical needs.
Efficiency & Adaptability Without Compromising Care
Swisscross demonstrates that humanitarian surgery can be both cost-efficient and high-quality. By focusing on targeted expertise—particularly in reconstructive surgery—and optimizing resources, the model ensures that care delivery is lean but impactful. Efficiency is not about doing less—it is about doing more with precision, ensuring that every intervention contributes to long-term outcomes rather than short-term output
Working in conflict and fragile settings requires flexibility. Swisscross teams operate beyond traditional surgical roles—functioning as clinicians, coordinators, and system-builders simultaneously. This adaptability allows integration into local health systems, rapid response to shifting conditions and better alignment with on-the-ground realities.
Rather than operating in isolation, Swisscross engages with broader networks of local stakeholders—clinicians, researchers, policymakers, and engineers—to co-create solutions.
This reflects a critical shift: humanitarian surgery is no longer a standalone activity, but part of a connected ecosystem of care.
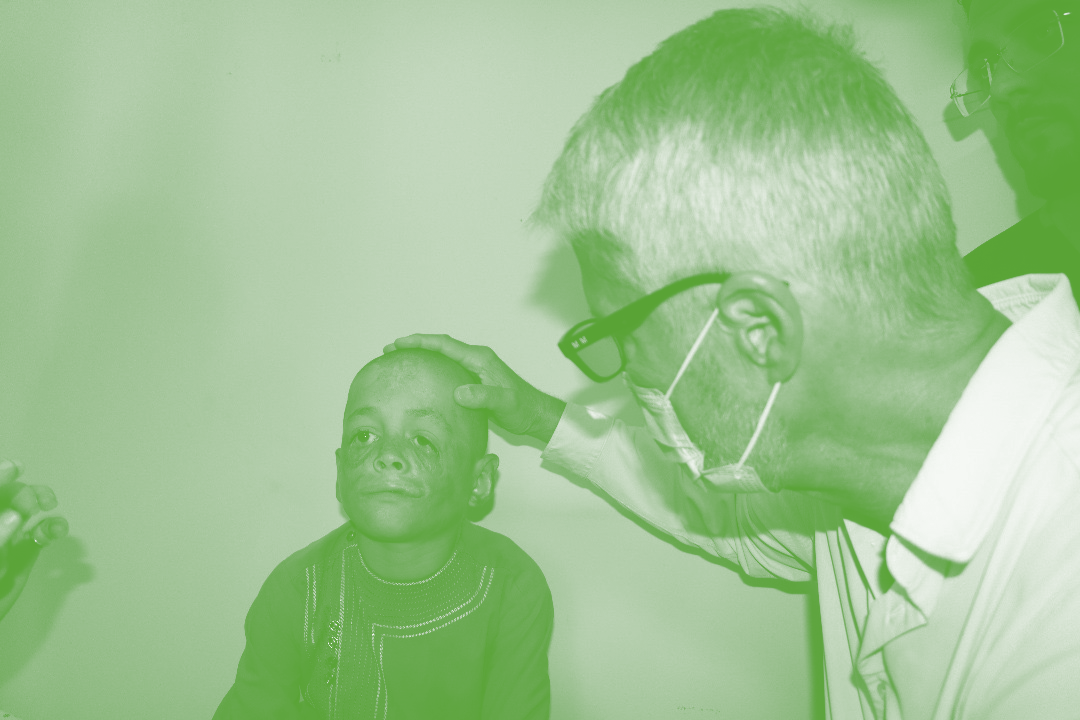
Swisscross Founder and Chair, Dr Enrique Steiger with a child with burn trauma in Kabul, Afghanistan.
The Next Frontier: A Globally Evolved Model
Building on approaches like Swisscross, the future of humanitarian surgery should rest on three pillars:
1. Locally Led Healthcare Systems
Sustainable impact requires shifting leadership to those closest to the need:
Local surgeons and providers become decision-makers
National systems are strengthened, not bypassed
International teams act as long-term partners
Success is no longer measured by how many surgeries are performed—but by how resilient the local system becomes.
2. Long-Term Capacity Building
The goal is not temporary relief, but lasting capability:
Training and mentorship embedded in every mission
Development of multidisciplinary surgical teams
Investment in infrastructure and education
This ensures that care continues long after international teams leave.
3. Technological Integration
Technology offers powerful tools to bridge gaps in access and expertise:
Telemedicine enabling remote collaboration
Digital systems improving continuity of care
Simulation and AI supporting training and planning
However, technology must remain context-appropriate.
In this new paradigm, international actors evolve from providers to partners, from surgeons to mentors, from operators to system enablers and from short-term responders to long-term collaborators.
Their legacy is not measured in procedures—but in capacity built and systems strengthened.
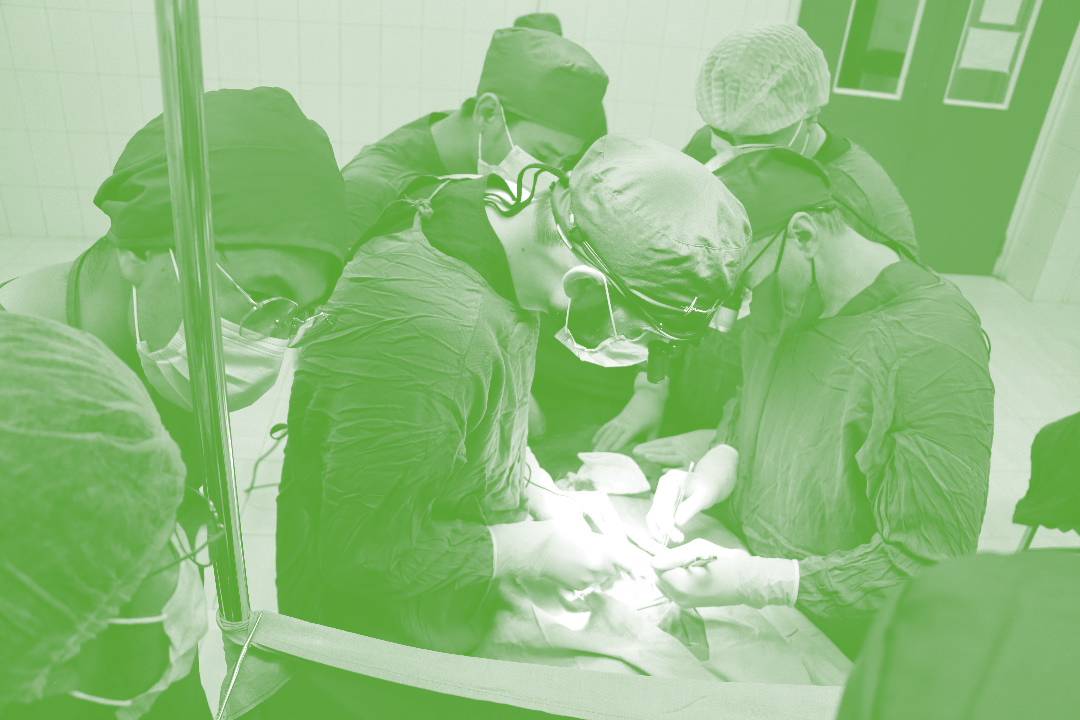
In one of the most fragile-settings like Afghanistan, Swisscross is working closely with local stakeholders to provide surgical care where it is needed most.
Building What Lasts
The future of humanitarian surgery is not just about scaling missions—it is about building systems.
It is a future where surgical care is consistently available within local systems, where healthcare professionals are empowered within their own communities and where global collaboration strengthens—not replaces—local capacity.
The Swisscross model offers a clear direction: efficient, effective, and empathetic care delivered through partnership and shared responsibility. The challenge now is to scale this mindset across the global health landscape. Because the true measure of humanitarian surgery is not what is done in a moment—
but what continues long after.
To support our work please donate.